Patient Sues Oral Surgeon After Unforeseeable Seizure
Marc Leffler, DDS, Esq.
July 28, 2025
Reading time: 8 minutes
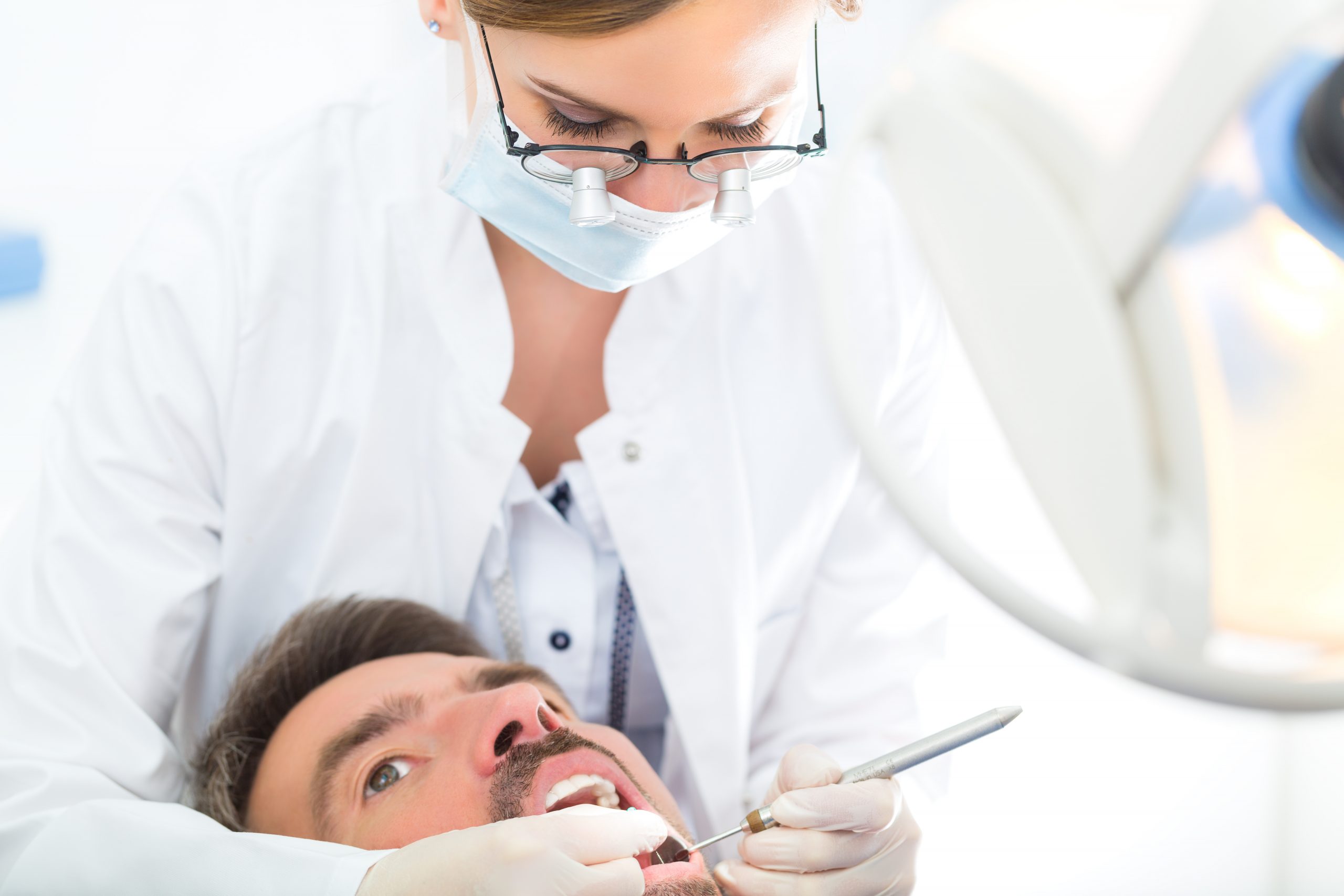
In oral surgery, medical emergencies, even if unforeseen, can still happen. In this case study, a patient presents to an oral surgeon for an implant placement procedure under local anesthesia. During the procedure, the patient suffers a grand mal seizure and is transported to a medical center for care. Later, the patient sues the oral surgeon for negligence, despite lacking medical evidence for the cause of the seizure.
Key Concepts
- Reasonable foreseeability in oral surgery
- Oral surgical guidelines and the standard of care
- Burden of proof in oral surgical malpractice litigation
Background Facts
Dr. H is a mid-career, experienced practitioner who has focused on implant dentistry for some years. J, a 50-year-old man with a disclosed history of hypertension, controlled with medication per his history, but no other known medical conditions, presented to Dr. H for her to place a single implant at the site of tooth #30, which had been lost 3 years prior due to a fracture. Radiographs demonstrated that the edentulous area had filled in well with bone that appeared to be of adequate volume and density to accommodate a fixture upon which a crown could eventually be placed.
A 13 mm implant was chosen to be placed into a radiographically-measured 15.5 mm space superior to the inferior alveolar canal. J saw no reason to be sedated for the procedure, as he had always been comfortable during a host of procedures performed under local anesthesia alone. After a thorough informed consent process took place, with written memorialization, Dr. H delivered a long buccal block as well as infiltrations, using 2 carpules of local anesthesia with epinephrine. J tolerated that well, with the area becoming anesthetized within a few minutes, as demonstrated by the lack of any response to a sharp instrument tested at various buccal and lingual locations.
After Dr. H elevated a soft tissue flap following a crestal incision, J became noticeably jittery and started to move around with “odd” opening and closing movements of the jaw, as Dr. H attempted the implant osteotomy. Dr. H briefly stopped work, but as she began again, the movements quickly progressed into what was clearly apparent as a grand mal seizure. Before she was able to stop the bur and remove the handpiece from the mouth, the osteotomy bur pierced through the buccal soft tissue and lower lip, on both sides of the commissure. With Dr. H’s assistance and instruction to her staff, the chairside assistant and Dr. H protected J from causing injury to himself and others, while the receptionist called for EMS.
By the time ambulance personnel arrived, the seizure had ended with J appearing to be in an altered state of awareness. Dr. H placed gauze over the lacerations and maintained hand pressure on them to minimize bleeding. J was then transported to a local medical center, where post-seizure care was provided and where oral and maxillofacial surgery residents repaired the lacerations, and debrided and closed the crestal incision.
J remained an in-patient for a complete neurological work-up, which never reached a conclusion as to the cause of the seizure. After returning home, he shortly resumed his usual activities while remaining under the watchful care of a neurologist. The scar which developed had a keloid appearance which bothered J greatly. Despite two scar revision procedures performed by a plastic surgeon, J was constantly self-conscious about his facial appearance, embarrassed to meet new people, both at work and in his social life.
Legal Action
J contacted a “malpractice law firm” whose poster he saw on a subway, wondering whether he might be able to be compensated for what he viewed as a physical deformity. The attorney assigned to handle J’s case soon advised J that he would be filing suit against Dr. H. After Dr. H was served and then assigned defense counsel by her malpractice carrier, the discovery process began. In the usual discovery paperwork, J, through his counsel, claimed that his facial scarring was directly caused by the negligence of Dr. H, namely that she had failed to protect him against the events which took place by having a proper finger rest, that she had failed to timely realize the prodromal stage of the seizure and to act upon that, and in delivering an excess amount of local anesthesia so as to cause the seizure.
The attorneys for Dr. H gathered all of J’s current and prior medical records, with particular focus on J’s post-seizure neurology work-up. They took specific note of the facts that J’s past medical history was as he had described it, and that the neurologist was unable to determine the cause of the seizure.
Armed with this information, as well as the expert affidavits of a dentist, an oral and maxillofacial surgeon, and a neurologist, they sought immediate dismissal of the case by way of a legal approach known as a motion for summary judgment (MSJ). In those MSJ papers, the defense attorneys argued, with the back-up of the experts, that no finger rest could have possibly prevented the seizure from occurring, and without the seizure, there would have been no laceration to develop into a keloid; that seizure prodromal stages are individual to every patient, and with no seizure history, Dr. H could not possibly have foreseen a potential seizure – no less know this patient’s prodromal signs – so as to interpret “odd” movements as being the onset of a seizure; that the amount of local anesthetic was far from excessive; and finally, but perhaps most important, that without a medically-known cause for the seizure, the case cannot legally stand.
In opposition, J’s attorney obtained his own experts, who, in essence, claimed that the adequacy of the finger rest, the lack of timely realization of the seizure prodome (so as to more quickly remove the bur from the mouth), and the amount of local anesthetic given, should be factual matters left for a jury, rather than legal matters to be determined before trial by a judge. Interestingly and tellingly, J’s opposition did not address the unknown cause for the seizure at all. However, it did add in the claim that Dr. H did not take J’s blood pressure prior to the treatment, in direct contravention of recent guidelines distributed by national organized oral surgery.
With the court having read all of the motion papers, at the close of oral arguments by both counsel before the court, the case was dismissed in its entirety. The court acknowledged that there could reasonably be disagreement as to whether Dr. H acted appropriately or negligently regarding the adequacy of the finger rest, or her noticing and acting on an impending seizure, or in how much local she delivered, or even in not measuring the patient’s pre-procedure blood pressure. But there could be no disagreement, the court reasoned, that there was no non-speculative way for a jury to conclude that any such negligence was the direct cause of the seizure, because no medical cause for the seizure – whether negligent or otherwise – had ever been determined.
Takeaways
For a plaintiff to be successful in an oral surgical malpractice case, the burden squarely falls on them to prove that (1) there was negligence on the part of the doctor (2) which directly caused (3) the injury complained-of. Failure to prove any one of those three elements is fatal to the claim. Consequently, a defendant need only disrupt any one of those elements to be successful in defense. Here, it was the judge, prior to trial, who determined that the “causation element” could not be proven by the plaintiff, because, without any medical evidence of the cause of the seizure, the claim that Dr. H’s negligence caused it was pure [legally unsound] speculation. In most cases, it is the jury that goes through a similar assessment, although based on the facts rather than legal principles, as to each of the required elements. And without that causation element proven – or as here, even able to be proven – the defendant oral surgeon prevailed, even though she might have arguably been negligent in some aspect of her care. Such is the world of law.
A motion for summary judgment is premised upon a lack of dispute, as to at least one of the required-to-be-proven case elements, between the parties. Therefore, a motion for summary judgment, when submitted by a defendant, need only demonstrate that at least one of the required elements cannot be met by the plaintiff. Here, Dr. H’s attorneys demonstrated to the court that the element of causation could not possibly be met by the plaintiff, warranting immediate, pre-trial dismissal. The court agreed.
The issue of the lack of the measuring of J’s blood pressure by Dr. H raises a few considerations. First of all, while it is true, as plaintiff contends, that guidelines do exist which suggest the taking of a patient’s blood pressure before every invasive procedure, those guidelines do not represent the standard of care, a concept that oral surgical organizations are quick to point out when issuing guidelines. But even if this court had accepted the guidelines as being the equivalent of standard of care, there was no medical evidence that an elevated blood pressure was the cause of this seizure, as previously discussed. The same can be said regarding the propriety or excessiveness of anesthetic dose, because, once again, the inability of the plaintiff to prove the causation element was fatal to his case.
Finally, we briefly discuss the concept of foreseeability, which is no stranger to issues determined by courts. Perhaps it is more accurate to speak about “foreseeability” as “reasonable foreseeability.” There are so many medical conditions and potential medical conditions that afflict patients, that it would be nearly impossible to foresee every medical problem that might come to pass on any given patient. So, while it is readily seen as reasonably foreseeable that even a well-controlled diabetic might suffer from a hypo- or hyper-glycemic event during a procedure, that same level of reasonableness does not exist so as to foresee a grand mal seizure in a patient with no seizure or neurologic history whatsoever. Yes, courts will often hold practitioners liable for foreseeable events, but that is generally interpreted as reasonably foreseeable events. The takeaway here is when you hear hoof beats, think horses, not zebras.
Additional Risk Tips content
OMS “Soft Sells” Risks of TMJ Surgery for A Locked Open Mandible
In this case study, a patient files a malpractice claim tied to informed consent, despite a successful surgery. Learn how communication affects risk.

Oral Surgeon Navigates the Gray Areas of Cosmetic Care
In this case study, a cosmetic facial treatment leads to a Board complaint against an OMS. Read the case to learn how scope of practice rules affect OMS.
Failure to Verify Leads to Irreversible Surgical Error
In this case study, wrong site oral surgery leads to malpractice claims. Read the article to learn how pre-procedure safeguards can prevent devastating errors.
This document does not constitute legal or medical advice and should not be construed as rules or establishing a standard of care. Because the facts applicable to your situation may vary, or the laws applicable in your jurisdiction may differ, please contact your attorney or other professional advisors if you have any questions related to your legal or medical obligations or rights, state or federal laws, contract interpretation, or other legal questions.
MedPro Group is the marketing name used to refer to the insurance operations of The Medical Protective Company, Princeton Insurance Company, PLICO, Inc. and MedPro RRG Risk Retention Group. All insurance products are underwritten and administered by these and other Berkshire Hathaway affiliates, including National Fire & Marine Insurance Company. Product availability is based upon business and/or regulatory approval and/or may differ among companies.
© MedPro Group Inc. All rights reserved.