Risk Associated with Cosmetic Procedures
July 2025
Reading time: 4 minutes
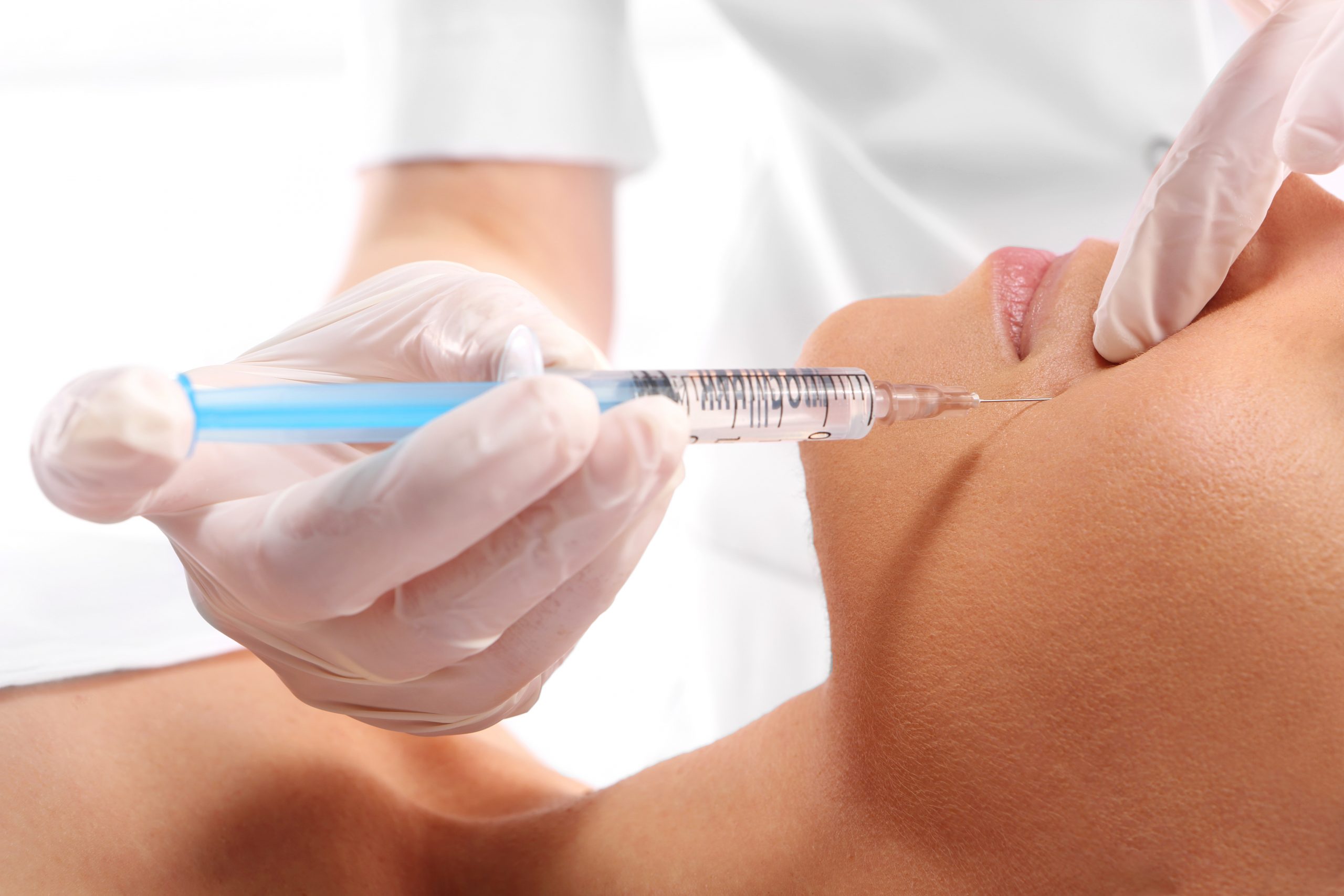
Managing patient expectations and providing clear, accurate information about care and treatment is an essential risk management strategy for practices. Failure to do so might increase the risk of patient complaints, requests for refunds, and even litigation. The need to manage patient expectations is particularly important when patients seek elective cosmetic treatment.
Oral and Maxillofacial Surgeons (OMS) who provide cosmetic services need to be confident that their patients have a realistic understanding about the results of treatment. Most providers of cosmetic services are aware that litigation may still occur — even when the clinical outcome was satisfactory — because the patient anticipated a different result.
Patient Misperceptions
Several factors contribute to patient misperceptions about cosmetic procedures. First, the desire to maximize one’s appearance is a highly emotional issue, and some patients expect that a cosmetic treatment or procedure will make them radiantly beautiful rather than simply address a particular cosmetic challenge.
Second, many cosmetic procedures aren’t covered by insurance, so patients must make significant financial investments to obtain these procedures or treatments. As a result, some patients find it difficult to accept the possibility that the results may be less than stellar.
Third, some patients are not merely seeking to improve their appearances; they are really trying to overhaul their identities. When such patients discover that — regardless of the clinical results — they must still deal with the same personal issues, their disappointment may be both illogical and unrelenting.
Finally, the OMS and staff need to be sensitive to the possibility that patients may recall promises and optimistic predictions rather than discussions about risks and limitations. Therefore, the importance of informed consent in the cosmetic environment cannot be overstated.
Promises are Risky
OMS must be especially careful that their advertising and marketing strategies don’t promise more than they can deliver. When in the market for “self-improvement,” some prospective patients hear only what they want to hear. For this reason, marketing strategies often are designed to promise emotional rather than physical results.
Examples of slogans that perpetuate emotional promises include:
- “Lose years by improving your smile!”
- “A whole new smile — a whole new outlook on life!”
- “Get the appearance you deserve!”
- “Straight teeth — new confidence!”
None of these slogans offer a physical result; rather, they promise an idealized “happy ever after.” This type of advertising may draw in potential clients, but it also may attract some people whose vision of change is impossible for even the most talented practitioner to help them achieve.
Advertising and Marketing Liability
OMS should carefully assess all prospective ads, signs, and brochures designed to sell their services. When reviewing these materials, OMS and staff alike should ask the following questions:
- Will this advertisement attract patients who have realistic expectations?
- Will this advertisement require that we achieve an impossibly high standard of care?
- Does the language use superlatives, make promises that are unrealistic, or urge patients to judge the results by emotional rather than clinical standards? Does the language promise or imply absolute satisfaction?
- Do advertisements make critical statements about competitive approaches to the services being offered? Do these comments inadvertently hold the practitioner to a higher standard by comparison?
While advertising motivates a potential client to take action — for example, to buy a particular product or service — marketing strategies generally are designed to trigger initial interest and help individuals identify wants or needs. Marketing materials also may provide reassurance to a client that he/she has made a wise decision, thereby preventing the post decision guilt known as “buyers’ remorse.”
Those who provide cosmetic services should be careful to distinguish between marketing materials and educational materials. Educational materials should offer patients objective, clear information about the risks and benefits of proposed treatments.
Educational materials are an important component of informed consent. They help patients negotiate the sometimes difficult process of formulating their questions, and they give OMS the opportunity to clarify and respond to patients’ concerns. Liability exposure increases when educational materials are written in terms that maximize the projected outcome of a cosmetic treatment and gloss over its risks.
Further, employees of a cosmetic-focused practice — in their eagerness to contribute to the success of the practice — might inadvertently mislead patients by referring to the OMS’ skills or past outcomes with glowing terms that could lead patients to expect the same perfect results, regardless of their individual circumstances.
Practice administration should clarify for all members of the team why particular marketing approaches are acceptable and why other tactics are unacceptable.
Conclusion
Those who market themselves as providers of cosmetic services should be cognizant of the border between a promise of dedicated effort on the patient’s behalf and a promise that the patient will achieve a nebulous vision of perfection. Advertising and marketing materials should be reviewed for accuracy and for any unintended commitments or promises that might obligate the OMS to comply with a higher, and perhaps unachievable, standard of care.
Patient education materials should be devoid of marketing hyperbole. Their purpose is to help the patient understand the risks and benefits of a procedure, the treatment plan, and its aftermath, including the patient’s obligation to engage in certain home care procedures and follow-up appointments.
Patients will benefit from their OMS’ clear vision of what cosmetic procedures might be able to achieve — as well as candid evaluations of what they might not be able to deliver.
WP_Query Object
(
[query] => Array
(
[post_type] => post
[showposts] => 3
[post__not_in] => Array
(
[0] => 4201
)
[post_status] => publish
[has_password] =>
[cat] => 1365
)
[query_vars] => Array
(
[post_type] => post
[showposts] => 3
[post__not_in] => Array
(
[0] => 4201
)
[post_status] => publish
[has_password] =>
[cat] => 1365
[error] =>
[m] =>
[p] => 0
[post_parent] =>
[subpost] =>
[subpost_id] =>
[attachment] =>
[attachment_id] => 0
[name] =>
[pagename] =>
[page_id] => 0
[second] =>
[minute] =>
[hour] =>
[day] => 0
[monthnum] => 0
[year] => 0
[w] => 0
[category_name] => risk-tips
[tag] =>
[tag_id] =>
[author] =>
[author_name] =>
[feed] =>
[tb] =>
[paged] => 0
[meta_key] =>
[meta_value] =>
[preview] =>
[s] =>
[sentence] =>
[title] =>
[fields] => all
[menu_order] =>
[embed] =>
[category__in] => Array
(
)
[category__not_in] => Array
(
)
[category__and] => Array
(
)
[post__in] => Array
(
)
[post_name__in] => Array
(
)
[tag__in] => Array
(
)
[tag__not_in] => Array
(
)
[tag__and] => Array
(
)
[tag_slug__in] => Array
(
)
[tag_slug__and] => Array
(
)
[post_parent__in] => Array
(
)
[post_parent__not_in] => Array
(
)
[author__in] => Array
(
)
[author__not_in] => Array
(
)
[search_columns] => Array
(
)
[ignore_sticky_posts] =>
[suppress_filters] =>
[cache_results] => 1
[update_post_term_cache] => 1
[update_menu_item_cache] =>
[lazy_load_term_meta] => 1
[update_post_meta_cache] => 1
[posts_per_page] => 3
[nopaging] =>
[comments_per_page] => 50
[no_found_rows] =>
[order] => DESC
)
[tax_query] => WP_Tax_Query Object
(
[queries] => Array
(
[0] => Array
(
[taxonomy] => category
[terms] => Array
(
[0] => 1365
)
[field] => term_id
[operator] => IN
[include_children] => 1
)
)
[relation] => AND
[table_aliases:protected] => Array
(
[0] => wp_4_term_relationships
)
[queried_terms] => Array
(
[category] => Array
(
[terms] => Array
(
[0] => 1365
)
[field] => term_id
)
)
[primary_table] => wp_4_posts
[primary_id_column] => ID
)
[meta_query] => WP_Meta_Query Object
(
[queries] => Array
(
)
[relation] =>
[meta_table] =>
[meta_id_column] =>
[primary_table] =>
[primary_id_column] =>
[table_aliases:protected] => Array
(
)
[clauses:protected] => Array
(
)
[has_or_relation:protected] =>
)
[date_query] =>
[request] => SELECT SQL_CALC_FOUND_ROWS wp_4_posts.ID
FROM wp_4_posts LEFT JOIN wp_4_term_relationships ON (wp_4_posts.ID = wp_4_term_relationships.object_id)
WHERE 1=1 AND wp_4_posts.ID NOT IN (4201) AND (
wp_4_term_relationships.term_taxonomy_id IN (11)
) AND wp_4_posts.post_password = '' AND wp_4_posts.post_type = 'post' AND ((wp_4_posts.post_status = 'publish'))
GROUP BY wp_4_posts.ID
ORDER BY wp_4_posts.post_date DESC
LIMIT 0, 3
[posts] => Array
(
[0] => WP_Post Object
(
[ID] => 7943
[post_author] => 180159417
[post_date] => 2026-04-13 10:28:20
[post_date_gmt] => 2026-04-13 14:28:20
[post_content] =>
In this case study, a treatment for recurrent mandibular subluxation led to unexpected complications and a malpractice claim centered on informed consent. The case highlights the importance of thoroughly discussing realistic risks before oral and maxillofacial surgery.
Key Concepts
- Why successful outcomes do not eliminate malpractice risk
- Benefits of maintaining empathy as an OMS
- How patient expectations can influence malpractice outcomes
Background Facts
P, a healthy, petite 31-year-old elementary school teacher, presented to Dr. V, the oral and maxillofacial surgeon who had extracted her third molars when she was in college. Within the past 6 months, P had made 5 trips to a local hospital ER due to her mouth locking in an open position (subluxation) after widely yawning (twice) and after taking large bites into food (three times). Each time, the emergency physician was able to readily "relocate" her jaw into her normal occlusion, except that the most recent episode required that she be given an intravenous sedative for the treatment to be accomplished. That last episode led the treating doctor to suggest that she see an oral surgeon to find out whether anything could be done to eliminate the problem.
After hearing the history, Dr. V performed a clinical evaluation, but the problem could not be replicated. A radiographic study revealed that P's left coronoid process was very pronounced and elongated, compared to both the right side and to what Dr. V had seen on many radiographic views of TMJs in other patients in general. Due to the specific anatomic arrangement, Dr. V explained to his patient, using a skull to demonstrate, that when she opened wide, the condylar head would sometimes slip ahead of the coronoid process – likely due to some soft tissue laxity – but it was unable to work itself back into the fossa because the coronoid process was too long to get past.
Dr. V believed that open joint surgery would be the best approach, with two potential options: (1) "tighten" the soft tissues so that the condyle would be less likely to slip forward; or (2) reduce the height of the coronoid process – by way of a procedure known as a coronoidectomy – so that if the jaw did slip forward, it would easily be able to retreat into the fossa. When asked his opinion, Dr. V suggested the coronoidectomy because it would be a lasting solution over time, regardless of how lax the intra-joint soft tissues might become.
P was inclined to proceed that way but wanted to think about it after discussing the risks and concerns more deeply. Dr. V and P did just that. He initially talked about the surgical entry. While an intraoral approach was preferred for a variety of reasons, most significantly a reduced risk of nerve injury, he was concerned about limited access because of her very small stature. So, he would plan to enter extraorally, just in front of the ear. When P followed up regarding the concern for nerves, Dr. V simply stated that there were a number of nerves in the area which are often stretched in the surgical process but generally recover quickly and that, "rarely," the effects can be more longstanding if the nerve itself is "cut into to any significant extent." Dr. V gave P a copy of a "TMJ surgery consent form," which discussed the nerve risks almost verbatim, as well as various other concerns such as infection, delayed healing, scarring, bleeding and pain.
After a month of consideration, P called Dr. V to tell him that she wanted to go forward. He asked her to come to the office to discuss scheduling and other surgery details. P brought her signed consent form with her, and surgery was planned for three weeks later.
P had her procedure done under general anesthesia, in an ambulatory surgery unit. Dr. V removed what he described as a large portion of the coronoid process, and flattened the entire anterior part of the complex, so that the condyle was able to move freely. At her first post-operative office appointment, P's clearly visible complaint was that she could not close her left eye; Dr. V explained that "this is what we went over beforehand", but P became upset because she had not expected such a significant and unaesthetic result, based upon Dr. V's very casual and downplayed description prior to surgery. Dr. V told P to wait for a while, because all was likely to return to normal. It never did.
Legal Action
Although P's TMJ subluxation was no longer a problem, she was emotionally distressed about how her students stared at her eye and about how her social life was adversely impacted, to say nothing of the need for her to use eye drops daily and having a constant sense of dryness. She worked with a mental health therapist and then retained an attorney to look into and potentially file a lawsuit against Dr. V, the latter of which did come to pass.
As the case progressed through discovery, both P and Dr. V provided deposition testimony. Questions to both of them addressed their respective views of the informed consent process. Beyond that, Dr. V discussed his surgical technique, which P's attorney would later admit to the trial jury was "textbook." During trial, even P's expert oral surgeon could not point to any meaningful criticisms of Dr. V's performing of the surgery. But the issue of informed consent was another story altogether.
The focus of trial regarding the claim of lack of informed consent honed in on the specific language used by Dr. V in his back-and-forth discussion with P, and on the signed consent form itself. P told the jury that she would never have gone through this surgery had Dr. V fully disclosed the risk of what actually happened to her. She called it a "soft sell," meaning that, while the subject of some vague nerve injury was raised, the details of it were not, and the likelihood of it happening was made to sound minimal, almost as a throwaway.
Shortly after the jury was sent to deliberate, its members sent a note to the judge that they had determined the issue of liability (which would later be revealed as no negligence on the part of Dr. V), but they wanted to look at the signed consent form and hear read-backs of the testimony from P and Dr. V regarding the risks explained. The jury ultimately concluded that Dr. V did not adequately warn P of the realistic risk of a motor nerve injury, nor the ramifications if it did happen. An award was given to compensate P for her emotional injuries – as corroborated by her therapist – as well as the physical injuries in and around her eye.
Takeaways
As this case study illustrates, a plaintiff will be successful and able to receive a monetary award by proving, to a jury's satisfaction, any one (or more) of the stated claims. Here, even though the jury found that Dr. V had met the standard of care with regard to surgical technique, his patient was still successful in her case of malpractice against him, due to his failure to adequately inform P before she consented to go forward with surgery. Informed consent is best not viewed as a mere afterthought, but rather an integral aspect of care with at least legal importance equal to that of the procedure. It warrants thoroughness and transparency.
Far from unusual is for plaintiffs to make case claims that they were negatively impacted to the extent that their mental health suffered. Those allegations are often minimized or even dismissed by judges, for lack of support. But here, P's assertions in that regard were backed up by a mental health therapist. That same concept holds true for all claims in malpractice cases. A plaintiff must present actual support, often times in the way of expert corroboration, to even be allowed to be considered by juries, to say nothing about getting compensation from those juries.
An issue raised in this case was that of the various treatment options available to oral surgeons. Here, Dr. V thoroughly considered those options and reasoned his way to a conclusion that guided his entire approach. While his decision was clearly a judgment call, a solid risk-protective approach taken by Dr. V in this regard was that he undertook a weighing process founded in scientific bases. Judgment calls happen regularly in practice, so they can be expected to be questioned in litigation scenarios. But Monday-morning quarterbacking is best overcome by having had a thoughtful process from the start, so the choice can be justified to a jury.
Finally, as was later described, Dr. V's comment to P when she presented post-op with a facial palsy – that "this is what we went over beforehand" – was not received well by his patient. Whether Dr. V demonstrated a sense of empathy at the time or not cannot be definitively concluded because of its subjective nature, but the underlying point is significant: patients expect their doctors to be caring, interested, and empathetic. Retrospective assessments, to the extent they are reliable, show that patients who feel cared-for, closely followed, and not cast aside by their doctors are less likely to sue them, with all else being equal. Patient care is why everyone signed on to be a part of this profession.
Summary of Takeaways
- Even when TMJ surgery is performed appropriately, inadequate informed consent can result in malpractice liability if realistic risks are not clearly communicated.
- Minimizing or vaguely describing potential complications can lead to unmet patient expectations.
- OMS can reduce risk by maintaining clear, empathetic communication before and after surgery.
Note that this case presentation includes circumstances from several different closed cases, in order to demonstrate certain legal and risk management principles, and that identifying facts and personal characteristics were modified to protect identities. The content within is not the original work of MedPro Group but has been published with consent of the author. Nothing contained in this article should be construed as legal, medical, or dental advice. Because the facts applicable to your situation may vary, or the laws applicable in your jurisdiction may differ, please contact your personal or business attorney or other professional advisors if you have any questions related to your legal or medical obligations or rights, state or federal laws, contract interpretation, or other legal questions.
[post_title] => OMS “Soft Sells” Risks of TMJ Surgery for A Locked Open Mandible [post_excerpt] => [post_status] => publish [comment_status] => open [ping_status] => open [post_password] => [post_name] => oms-soft-sells-risks-of-tmj-surgery-for-a-locked-open-mandible [to_ping] => [pinged] => [post_modified] => 2026-04-24 12:58:09 [post_modified_gmt] => 2026-04-24 16:58:09 [post_content_filtered] => [post_parent] => 0 [guid] => https://oms.medprodental.com/?p=7943 [menu_order] => 0 [post_type] => post [post_mime_type] => [comment_count] => 0 [filter] => raw ) [1] => WP_Post Object ( [ID] => 7921 [post_author] => 180159417 [post_date] => 2026-03-29 22:55:44 [post_date_gmt] => 2026-03-30 02:55:44 [post_content] =>In this case study, oral and maxillofacial surgeons will learn how facial cosmetic injections performed under a dental license led to a Dental Board complaint and formal investigation. These events highlight the need for clarity around scope-of-practice boundaries and training requirements.
Key Concepts
- Risk of performing procedures without experience
- How patient dissatisfaction can lead to Board complaints
- Understanding State Dental Practice Acts
Background Facts
K, a healthy 32-year-old woman, had recently seen several of her friends and work colleagues receiving facial injections to enhance lip fullness and eliminate lines and wrinkles on their foreheads. She thought about undergoing procedures of those types, but she was very fearful of doctors in general. There was one exception to that: the oral surgeon who had removed her third molars some years back and had pleasantly surprised her with the ease of the procedure and its after-effects. K wondered whether Dr. N did those kinds of cosmetic treatments and was happy to learn from his office staff that he did. She made an appointment for a consultation.
Dr. N, an oral and maxillofacial surgeon, practiced under a dental license. At their office meeting, Dr. N explained to K that he would be able to inject dermal filler into her lips to "make them more plump" and inject one of the commonly used neuromuscular blocking agents to eliminate forehead lines. Dr. N explicitly pointed out that the beneficial effects would be temporary, on the order of months, or perhaps even a year or more. He also explained the traditional risks of both types of procedures. K's only concern was financial, but Dr. N's office worked out a payment plan to make that aspect of the picture easier for her.
Nearly a month after the consultation, K presented to Dr. N for the planned cosmetic treatments. The office procedures went without complication, with K discharged home with her accompanying friend a few hours later. When Dr. N called K the next day, she told him that she was swollen and red at all injection sites. She was assured that this was all normal. At her one-week post-treatment visit, she expressed her displeasure with the asymmetry of both of her lips. She was again assured that this was normal and that all would "equalize" shortly. In fact, the asymmetries did not resolve. Even approaching 18 months, the "lopsidedness" of the lips remained.
K met with a plastic surgeon to assess any corrective options she might have. The plastic surgeon had no criticisms regarding the forehead, but was quite critical of the lip results, stating that the amounts and locations of filler placement had to have been inappropriate. However, no surgical or other solutions were offered, absent simply waiting a few more months until the effects would almost certainly be gone.
Although it did come to pass that the effects were soon to dissipate, K had endured what she viewed as a particularly stressful period, during which her social life suffered, social media comments about her appearance regularly popped, and even work officemates murmured about. Despite her requests, K was given no credit on her remaining balance, so she eventually paid Dr. N in full.
Legal Action
Two attorneys refused K's potential malpractice case against Dr. N, both saying that the effects ended up being temporary, and explaining to K that they doubted a jury's sympathy regarding entirely cosmetic procedures, particularly during the difficult economic times in their location.
The latter issue resonated with K, in that she continued to harbor resentment about Dr. N's unwillingness to reduce the amount she owed him. She wondered aloud to one of the attorneys as to any other remedies that might be available and was told that she had the option of filing a Dental Board complaint against Dr. N. Wanting to at least "do something," she went down that path. The complaint itself merely set forth what treatments Dr. N had performed, asserting that they were done poorly. The Board sent a letter-request for copies of all records from Dr. N.
Dr. N reported the communication from the Board to his malpractice carrier, which assigned him counsel to assist in defending against the complaint. Counsel provided the Board with all that they requested and accompanied Dr. N to hearings before the members. The Board asked Dr. N detailed questions, about both the lip and forehead procedures, focusing on his experience and training, which had been rather limited.
The Board's findings against Dr. N were scathing, citing his training as inadequate – as it included only academic coursework – and his experience as having "not even worked with a skilled practitioner until he could develop expertise." The Board accepted Dr. N's explanation that the lip procedures had a dentally-based therapeutic purpose, namely reducing lip incompetence so as to improve such oral functions as eating, drinking and speaking. However, Dr. N was unable to provide an analogous basis for the forehead injections he had performed. As such, the Board concluded that his treatment had fallen outside of the permissible scope of practicing dentistry, per the State's Dental Practice Act, in that it was not performed to restore or maintain dental health (which the Board pointed out might have been the case had the patient had muscular-based conditions such as bruxism, TMD, or trismus, which was not the situation here).
Dr. N was sanctioned by the Board by way of fines, a suspension from practice (which was stayed), and a mandate to complete continuing education on jurisprudence in dental practice.
Takeaways
The various States have different and often unique provisions which guide and limit the practice of dentistry, and scope of practice is among those provisions. While oral surgeons are sometimes granted additional allowances as to increased scope of practice, that is not always the case. Therefore, prior to undertaking procedures which might go outside of the "traditional," it is wise to consult the State's Dental Practice Act and potentially speak with the authorities directly. This is particularly appropriate when an oral surgeon has offices on both sides of State borders, where the rules might be entirely different. As this case study demonstrates, the penalties for violations can be severe.
Patients who are dissatisfied with aspects of their care have multiple potential remedies at their disposals, even when, as here, the patient does not directly benefit from an outcome against the provider. Perhaps ironically, it was not the aspect of care by Dr. N that K was displeased about – her lips – that led to the Board's penalties. Dental Boards are free to delve through the entire patient record, despite a complaint about a limited issue, and levy penalties for any violation they might see, whether that was a patient concern or not.
As cliché as it might sound, angry patients are more likely to initiate lawsuits and Board complaints, with all else being equal regarding treatment results. In this case study, K was clearly unhappy with how the esthetics turned out, but it was Dr. N's unwillingness to adjust his fee that led her to take action. An argument can be made, although speculative, that K acted in a retributive way. Whether true or not, that is not an issue that the Board would likely consider. While we do not comment upon the charging or waiving of fees, this concept speaks to the importance of maintaining cordiality and professionalism at every step, to reduce the likelihood of patient complaints of all types.
The plastic surgeon who evaluated K after her treatment with Dr. N engaged in what we refer to as "jousting," which in simple terms is throwing another practitioner under the bus. Jousting is a significant driver of malpractice claims, so its implications cannot be overstated. When subsequent practitioners joust, they often fail to consider, or even know about, what the prior treating doctor faced regarding presenting conditions, patient aspirations, and patient-directed limitations, yet their statements nevertheless loom large to patients, and eventually to trial juries. The ethics of jousting are subjective and not an issue to be discussed here, but it is inescapable that many malpractice suits get off the ground simply because of it.
Stepping away from implications regarding malpractice suits and Board actions, but into the realm of direct patient care, practitioners best serve their patients when performing procedures for which they have been adequately and properly trained, didactically and clinically, so patients can obtain the best results available. That might be seen as something of a catch-22, in that all practitioners constantly learn, expand, and improve, which could very reasonably be hindered by a concern about venturing into new areas. This is a personal judgment call, with sometimes opposing issues needing to be weighed and acted upon. In the end, though, if a case ends up in litigation, and the defendant-doctor is asked questions at a deposition, it is fair game for plaintiff's counsel to explore all of these issues so that they can ultimately be considered by a trial jury.
Finally, we have intentionally omitted the names of the products used to treat K, to avoid any potential inferences about particular ones.
Summary of Takeaways
- Performing cosmetic procedures without clear alignment with the state’s scope of practice rules can expose OMS to significant Board scrutiny and disciplinary action.
- Even when patient harm is temporary, dissatisfaction can escalate into complaints that trigger broad regulatory review beyond the original concern.
- OMS can reduce risk by maintaining professionalism in patient interactions and by confirming their training, experience, and state’s rules before offering cosmetic care.
Note that this case presentation includes circumstances from several different closed cases, in order to demonstrate certain legal and risk management principles, and that identifying facts and personal characteristics were modified to protect identities. The content within is not the original work of MedPro Group but has been published with consent of the author. Nothing contained inthis article should be construed as legal, medical, or dental advice. Because the facts applicable to your situation may vary, or the laws applicable in your jurisdiction may differ, please contact your personal or business attorney or other professional advisors if you have any questions related to your legal or medical obligations or rights, state or federal laws, contract interpretation, or other legal questions.
[post_title] => Oral Surgeon Navigates the Gray Areas of Cosmetic Care [post_excerpt] => [post_status] => publish [comment_status] => open [ping_status] => open [post_password] => [post_name] => oral-surgeon-navigates-the-gray-areas-of-cosmetic-care [to_ping] => [pinged] => [post_modified] => 2026-04-28 15:38:12 [post_modified_gmt] => 2026-04-28 19:38:12 [post_content_filtered] => [post_parent] => 0 [guid] => https://oms.medprodental.com/?p=7921 [menu_order] => 0 [post_type] => post [post_mime_type] => [comment_count] => 0 [filter] => raw ) [2] => WP_Post Object ( [ID] => 7898 [post_author] => 180159417 [post_date] => 2026-03-04 06:30:26 [post_date_gmt] => 2026-03-04 11:30:26 [post_content] =>In this case study, oral and maxillofacial surgeons (OMS) will examine how a documentation error and failure to clinically verify a biopsy site led to wrong site oncologic surgery and malpractice claims. The case highlights the importance of obtaining clinical clarity before procedures.
Key Concepts
- Preventing wrong-site surgery through pre-procedure precautions
- Vicarious liability for documentation errors
- Pure consent to settle clauses in malpractice policies
Background Facts
T, a 71-year-old man, was a retired carpenter, with a history of well-controlled hypertension and chronic, episodic sinusitis, and having smoked at various times in his life, as much as a pack of cigarettes a day. He visited his dentist, Dr. D, at irregular intervals and never wanted to establish a big-picture treatment plan. At his most recent visit, Dr. D noted a course, irregular white area at the buccal mucogingival junction around teeth #29-31. Not feeling comfortable making a provisional diagnosis, Dr. D referred T to a periodontist, Dr. O, to evaluate the area and treat as needed. Dr. O performed an incisional biopsy of the area and sent it to an oral pathologist, Dr. H, for histopathological assessment. The lesion was read out provisionally as atypical epithelial proliferation, but Dr. H asked for a larger sample to be able to make a more definitive diagnosis.
Dr. O took a second specimen from an immediately adjacent site. Due to a clerical error, Dr. O entered into the chart that this specimen had been taken from the "lower left buccal gingiva," with her dental assistant repeating that error on the pathology request form that was forwarded to Dr. H with the tissue. After microscopically examining the specimen, Dr. H diagnosed it definitively. The report from Dr. H to Dr. O read "squamous cell carcinoma, moderately-to-well differentiated, lower left buccal gingiva," the latter aspect having been copied by Dr. H, exactly from the requisition provided by Dr. O's office with the most recent submission.
Upon seeing the words "squamous cell carcinoma," Dr. O immediately referred T to a double-degree oral and maxillofacial surgeon, Dr. M, who had head-and-neck surgery fellowship training, for evaluation and treatment, giving T a copy of the biopsy report to take with him. Dr. M reviewed Dr. H's report, examined T, noting a small lesion on the buccal aspect of teeth #30-31, and explained to T that he would need a PET scan to determine whether there had been any spread. Presuming no such spread, Dr. M advised T that the lesion could be successfully treated by surgery alone, specifically a marginal mandibulectomy and a limited neck dissection. The lesion had not spread, per the PET scan and other modalities, so the stated plan would go forward. T agreed and surgery was scheduled at a regional medical center.
On the day of surgery, T waited in a pre-surgery room, where his medical history was reviewed and identification was checked. A consent form stating the procedure to be "removal of portion of lower jaw, and neck dissection" was signed by T and witnessed by a nurse. Dr. M said a brief "hello" to T before changing into scrubs and entering the operating room, where T was already on the table. Dr. M asked the anesthesiologist to proceed.
Dr. M had taped Dr. H's biopsy report to the OR wall, read it again, and prepared to make an extraoral left submandibular incision, through which he would both remove a mandibular segment and perform the limited neck dissection. Technically, the procedure went forward uneventfully, with T then transferred to the post-anesthesia care unit. T's wife was brought in to see her husband while Dr. M was still there, dictating his operative note. She was aghast to see that surgery had been performed on T's left side, when she knew that the cancer was on the right. When she confronted Dr. M on the spot, he said, "here's the biopsy report, read it for yourself."
Shortly after T's initial surgical recovery, another surgeon treated T, this time correctly operating on the right side of T's face and neck. T suffered emotionally, to the extent that he sought and obtained psychological counseling, but he was never able to comfortably eat or drink, or otherwise normally function orally again. He required and received reconstruction bilaterally, but he always found it to be very compromised and esthetically unacceptable.
Legal Action
T retained a seasoned attorney, who collected all records and obtained opinions from a general dentist (like Dr. D), a periodontist (like Dr. O), an oral pathologist (like Dr. H), and an OMS (like Dr. M). The general dentist saw no liability on Dr. D's part, as he had immediately made an appropriate referral. The oral pathologist similarly found no liability as to Dr. H, reasoning that oral pathologists in biopsy situations do not assess the patient clinically. They simply diagnose what they see microscopically, which he did accurately, and report the findings regarding the site that was conveyed on the requisition it had come from.
The conclusions as to Drs. O and M were quite the different. The expert periodontist stated his view of Dr. O's negligence succinctly: Dr. O's recording error which incorrectly stated the location of the lesion to be examined was inexcusable, and it served to set the entire cascade of events into action, resulting in wrong-side surgery having been done. The oral surgery expert was deeply critical of Dr. M, claiming that he failed to clinically correlate the location findings on a biopsy report with the patient's actual condition, and then compounded the situation by being unwilling to address his error, thereby violating his duties, both surgically and ethically. In short, said this expert, Dr. M failed to do the most basic tasks, namely double checking the intended surgical site before performing irreversible, life-altering treatments.
Substantial settlement amounts were paid to T on behalf of both Dr. O and Dr. M. Additionally, Dr. M was sanctioned by his State Board.
Takeaways
Wrong-site treatment, including surgery – whether, as here, relating to the side of the mandible to be removed, or extracting a first bicuspid instead of an orthodontically planned-for second bicuspid, or endodontically treating a healthy lower molar instead of the diseased tooth next to it – has permanent effects, which are virtually always preventable. Pre-procedure techniques can be, and routinely are, employed that will stop this type of error from ever taking place, such as taking a time out for confirmation, marking the side/site of surgery, having two people independently confirm what is to be done, clinically correlating a result document (such as a biopsy report) with an actual finding, and having an open, no-consequences policy that encourages office staff to voice any concerns before a potential untoward event begins. The old "a stitch in time" adage is never more applicable than in pre-procedure risk protection.
One of the most frequent case types now seen in malpractice claims is a practitioner performing treatment where it was not intended to be, and the trend appears to be growing. While the reasons for that are simply theories, a common-sense approach is that such events might well be driven by a focus on the number of patients seen and procedures performed. In reality, the amount of time needed before a procedure to assure correct patient, correct site, correct procedure is nominal in comparison to the amount of time that most procedures take. But even if a practitioner or an office is measurably slowed down to achieve those assurances, obligations to patient safety warrant those delays.
This case highlights the consideration of responding to patients and their family members when results are not as planned or expected, when complications come to pass, or, as here, when errors are immediately obvious. It would not likely have changed the ultimate course of legal events had Dr. M responded to T's wife differently, because the negligence was so clear and significant, but it might have reduced the likelihood of a Board complaint being levied against him. Evidence to support that theory lies with the fact that no Board complaint was filed against Dr. O.
The pathology request form sent to Dr. H with the second specimen taken by Dr. O was completed by Dr. O's dental assistant, who wrote the requisition form. By way of a concept known as vicarious liability, what the dental assistant wrote is the functional equivalent of Dr. O having written it herself. The assistant's error, whether copied from Dr. O's own transcription error or not, becomes Dr. O's error as well. All that is delegated comes back to the delegator, so double-checking of even such a seemingly unimportant task is critical for liability protection and for patient protection.
As a background fact, both Dr. O and Dr. M had professional liability ("dental malpractice") policies with "pure consent-to-settle" provisions, meaning that no settlement could have been reached without their agreement to do so. Such a provision means that a practitioner can demand that a lawsuit brought against them be tried in court before a jury, regardless of how strong the evidence of wrongdoing might be. For every case, practitioners are counseled by their attorneys regarding the pros and cons of settlement versus trial, with the potential implications of both fully set out on the table.
Finally, we note that, simply for purposes of brevity, some details, which were not relevant to the risk management issues discussed, were omitted. This is particularly the case regarding the pre-surgical work-up phase of care, secondary criticisms addressed by the experts, and the documentary and testimonial evidence before the State Board. Their absence should not be construed as necessary but missing pieces.
Summary of Takeaways
- Wrong site surgery remains a leading and largely preventable source of malpractice claims.
- OMS are accountable for errors made by delegated staff, even when those errors were unintentional.
- Simple confirmation practices before irreversible procedures can prevent patient harm and legal consequences.
Note that this case presentation includes circumstances from several different closed cases, in order to demonstrate certain legal and risk management principles, and that identifying facts and personal characteristics were modified to protect identities. The content within is not the original work of MedPro Group but has been published with consent of the author. Nothing contained in this article should be construed as legal, medical, or dental advice. Because the facts applicable to your situation may vary, or the laws applicable in your jurisdiction may differ, please contact your personal or business attorney or other professional advisors if you have any questions related to your legal or medical obligations or rights, state or federal laws, contract interpretation, or other legal questions.
[post_title] => Failure to Verify Leads to Irreversible Surgical Error [post_excerpt] => [post_status] => publish [comment_status] => open [ping_status] => open [post_password] => [post_name] => missed-verification-leads-to-irreversible-surgical-error [to_ping] => [pinged] => [post_modified] => 2026-05-01 09:22:09 [post_modified_gmt] => 2026-05-01 13:22:09 [post_content_filtered] => [post_parent] => 0 [guid] => https://oms.medprodental.com/?p=7898 [menu_order] => 0 [post_type] => post [post_mime_type] => [comment_count] => 0 [filter] => raw ) ) [post_count] => 3 [current_post] => -1 [before_loop] => 1 [in_the_loop] => [post] => WP_Post Object ( [ID] => 7943 [post_author] => 180159417 [post_date] => 2026-04-13 10:28:20 [post_date_gmt] => 2026-04-13 14:28:20 [post_content] =>In this case study, a treatment for recurrent mandibular subluxation led to unexpected complications and a malpractice claim centered on informed consent. The case highlights the importance of thoroughly discussing realistic risks before oral and maxillofacial surgery.
Key Concepts
- Why successful outcomes do not eliminate malpractice risk
- Benefits of maintaining empathy as an OMS
- How patient expectations can influence malpractice outcomes
Background Facts
P, a healthy, petite 31-year-old elementary school teacher, presented to Dr. V, the oral and maxillofacial surgeon who had extracted her third molars when she was in college. Within the past 6 months, P had made 5 trips to a local hospital ER due to her mouth locking in an open position (subluxation) after widely yawning (twice) and after taking large bites into food (three times). Each time, the emergency physician was able to readily "relocate" her jaw into her normal occlusion, except that the most recent episode required that she be given an intravenous sedative for the treatment to be accomplished. That last episode led the treating doctor to suggest that she see an oral surgeon to find out whether anything could be done to eliminate the problem.
After hearing the history, Dr. V performed a clinical evaluation, but the problem could not be replicated. A radiographic study revealed that P's left coronoid process was very pronounced and elongated, compared to both the right side and to what Dr. V had seen on many radiographic views of TMJs in other patients in general. Due to the specific anatomic arrangement, Dr. V explained to his patient, using a skull to demonstrate, that when she opened wide, the condylar head would sometimes slip ahead of the coronoid process – likely due to some soft tissue laxity – but it was unable to work itself back into the fossa because the coronoid process was too long to get past.
Dr. V believed that open joint surgery would be the best approach, with two potential options: (1) "tighten" the soft tissues so that the condyle would be less likely to slip forward; or (2) reduce the height of the coronoid process – by way of a procedure known as a coronoidectomy – so that if the jaw did slip forward, it would easily be able to retreat into the fossa. When asked his opinion, Dr. V suggested the coronoidectomy because it would be a lasting solution over time, regardless of how lax the intra-joint soft tissues might become.
P was inclined to proceed that way but wanted to think about it after discussing the risks and concerns more deeply. Dr. V and P did just that. He initially talked about the surgical entry. While an intraoral approach was preferred for a variety of reasons, most significantly a reduced risk of nerve injury, he was concerned about limited access because of her very small stature. So, he would plan to enter extraorally, just in front of the ear. When P followed up regarding the concern for nerves, Dr. V simply stated that there were a number of nerves in the area which are often stretched in the surgical process but generally recover quickly and that, "rarely," the effects can be more longstanding if the nerve itself is "cut into to any significant extent." Dr. V gave P a copy of a "TMJ surgery consent form," which discussed the nerve risks almost verbatim, as well as various other concerns such as infection, delayed healing, scarring, bleeding and pain.
After a month of consideration, P called Dr. V to tell him that she wanted to go forward. He asked her to come to the office to discuss scheduling and other surgery details. P brought her signed consent form with her, and surgery was planned for three weeks later.
P had her procedure done under general anesthesia, in an ambulatory surgery unit. Dr. V removed what he described as a large portion of the coronoid process, and flattened the entire anterior part of the complex, so that the condyle was able to move freely. At her first post-operative office appointment, P's clearly visible complaint was that she could not close her left eye; Dr. V explained that "this is what we went over beforehand", but P became upset because she had not expected such a significant and unaesthetic result, based upon Dr. V's very casual and downplayed description prior to surgery. Dr. V told P to wait for a while, because all was likely to return to normal. It never did.
Legal Action
Although P's TMJ subluxation was no longer a problem, she was emotionally distressed about how her students stared at her eye and about how her social life was adversely impacted, to say nothing of the need for her to use eye drops daily and having a constant sense of dryness. She worked with a mental health therapist and then retained an attorney to look into and potentially file a lawsuit against Dr. V, the latter of which did come to pass.
As the case progressed through discovery, both P and Dr. V provided deposition testimony. Questions to both of them addressed their respective views of the informed consent process. Beyond that, Dr. V discussed his surgical technique, which P's attorney would later admit to the trial jury was "textbook." During trial, even P's expert oral surgeon could not point to any meaningful criticisms of Dr. V's performing of the surgery. But the issue of informed consent was another story altogether.
The focus of trial regarding the claim of lack of informed consent honed in on the specific language used by Dr. V in his back-and-forth discussion with P, and on the signed consent form itself. P told the jury that she would never have gone through this surgery had Dr. V fully disclosed the risk of what actually happened to her. She called it a "soft sell," meaning that, while the subject of some vague nerve injury was raised, the details of it were not, and the likelihood of it happening was made to sound minimal, almost as a throwaway.
Shortly after the jury was sent to deliberate, its members sent a note to the judge that they had determined the issue of liability (which would later be revealed as no negligence on the part of Dr. V), but they wanted to look at the signed consent form and hear read-backs of the testimony from P and Dr. V regarding the risks explained. The jury ultimately concluded that Dr. V did not adequately warn P of the realistic risk of a motor nerve injury, nor the ramifications if it did happen. An award was given to compensate P for her emotional injuries – as corroborated by her therapist – as well as the physical injuries in and around her eye.
Takeaways
As this case study illustrates, a plaintiff will be successful and able to receive a monetary award by proving, to a jury's satisfaction, any one (or more) of the stated claims. Here, even though the jury found that Dr. V had met the standard of care with regard to surgical technique, his patient was still successful in her case of malpractice against him, due to his failure to adequately inform P before she consented to go forward with surgery. Informed consent is best not viewed as a mere afterthought, but rather an integral aspect of care with at least legal importance equal to that of the procedure. It warrants thoroughness and transparency.
Far from unusual is for plaintiffs to make case claims that they were negatively impacted to the extent that their mental health suffered. Those allegations are often minimized or even dismissed by judges, for lack of support. But here, P's assertions in that regard were backed up by a mental health therapist. That same concept holds true for all claims in malpractice cases. A plaintiff must present actual support, often times in the way of expert corroboration, to even be allowed to be considered by juries, to say nothing about getting compensation from those juries.
An issue raised in this case was that of the various treatment options available to oral surgeons. Here, Dr. V thoroughly considered those options and reasoned his way to a conclusion that guided his entire approach. While his decision was clearly a judgment call, a solid risk-protective approach taken by Dr. V in this regard was that he undertook a weighing process founded in scientific bases. Judgment calls happen regularly in practice, so they can be expected to be questioned in litigation scenarios. But Monday-morning quarterbacking is best overcome by having had a thoughtful process from the start, so the choice can be justified to a jury.
Finally, as was later described, Dr. V's comment to P when she presented post-op with a facial palsy – that "this is what we went over beforehand" – was not received well by his patient. Whether Dr. V demonstrated a sense of empathy at the time or not cannot be definitively concluded because of its subjective nature, but the underlying point is significant: patients expect their doctors to be caring, interested, and empathetic. Retrospective assessments, to the extent they are reliable, show that patients who feel cared-for, closely followed, and not cast aside by their doctors are less likely to sue them, with all else being equal. Patient care is why everyone signed on to be a part of this profession.
Summary of Takeaways
- Even when TMJ surgery is performed appropriately, inadequate informed consent can result in malpractice liability if realistic risks are not clearly communicated.
- Minimizing or vaguely describing potential complications can lead to unmet patient expectations.
- OMS can reduce risk by maintaining clear, empathetic communication before and after surgery.
Note that this case presentation includes circumstances from several different closed cases, in order to demonstrate certain legal and risk management principles, and that identifying facts and personal characteristics were modified to protect identities. The content within is not the original work of MedPro Group but has been published with consent of the author. Nothing contained in this article should be construed as legal, medical, or dental advice. Because the facts applicable to your situation may vary, or the laws applicable in your jurisdiction may differ, please contact your personal or business attorney or other professional advisors if you have any questions related to your legal or medical obligations or rights, state or federal laws, contract interpretation, or other legal questions.
[post_title] => OMS “Soft Sells” Risks of TMJ Surgery for A Locked Open Mandible [post_excerpt] => [post_status] => publish [comment_status] => open [ping_status] => open [post_password] => [post_name] => oms-soft-sells-risks-of-tmj-surgery-for-a-locked-open-mandible [to_ping] => [pinged] => [post_modified] => 2026-04-24 12:58:09 [post_modified_gmt] => 2026-04-24 16:58:09 [post_content_filtered] => [post_parent] => 0 [guid] => https://oms.medprodental.com/?p=7943 [menu_order] => 0 [post_type] => post [post_mime_type] => [comment_count] => 0 [filter] => raw ) [comment_count] => 0 [current_comment] => -1 [found_posts] => 58 [max_num_pages] => 20 [max_num_comment_pages] => 0 [is_single] => [is_preview] => [is_page] => [is_archive] => 1 [is_date] => [is_year] => [is_month] => [is_day] => [is_time] => [is_author] => [is_category] => 1 [is_tag] => [is_tax] => [is_search] => [is_feed] => [is_comment_feed] => [is_trackback] => [is_home] => [is_privacy_policy] => [is_404] => [is_embed] => [is_paged] => [is_admin] => [is_attachment] => [is_singular] => [is_robots] => [is_favicon] => [is_posts_page] => [is_post_type_archive] => [query_vars_hash:WP_Query:private] => c74a42a892d6636102c1e70e6c888782 [query_vars_changed:WP_Query:private] => [thumbnails_cached] => [allow_query_attachment_by_filename:protected] => [stopwords:WP_Query:private] => [compat_fields:WP_Query:private] => Array ( [0] => query_vars_hash [1] => query_vars_changed ) [compat_methods:WP_Query:private] => Array ( [0] => init_query_flags [1] => parse_tax_query ) [query_cache_key:WP_Query:private] => wp_query:d73e803f6ea31df43c081d05758aa4cf )Additional Risk Tips content
OMS “Soft Sells” Risks of TMJ Surgery for A Locked Open Mandible
In this case study, a patient files a malpractice claim tied to informed consent, despite a successful surgery. Learn how communication affects risk.

Oral Surgeon Navigates the Gray Areas of Cosmetic Care
In this case study, a cosmetic facial treatment leads to a Board complaint against an OMS. Read the case to learn how scope of practice rules affect OMS.
Failure to Verify Leads to Irreversible Surgical Error
In this case study, wrong site oral surgery leads to malpractice claims. Read the article to learn how pre-procedure safeguards can prevent devastating errors.
This document does not constitute legal or medical advice and should not be construed as rules or establishing a standard of care. Because the facts applicable to your situation may vary, or the laws applicable in your jurisdiction may differ, please contact your attorney or other professional advisors if you have any questions related to your legal or medical obligations or rights, state or federal laws, contract interpretation, or other legal questions.
MedPro Group is the marketing name used to refer to the insurance operations of The Medical Protective Company, Princeton Insurance Company, PLICO, Inc. and MedPro RRG Risk Retention Group. All insurance products are underwritten and administered by these and other Berkshire Hathaway affiliates, including National Fire & Marine Insurance Company. Product availability is based upon business and/or regulatory approval and/or may differ among companies.
© MedPro Group Inc. All rights reserved.