Patient Sues OMS for Malocclusion Treatment Errors
Marc Leffler, DDS, Esq.
July 28, 2025
Reading time: 8 minutes
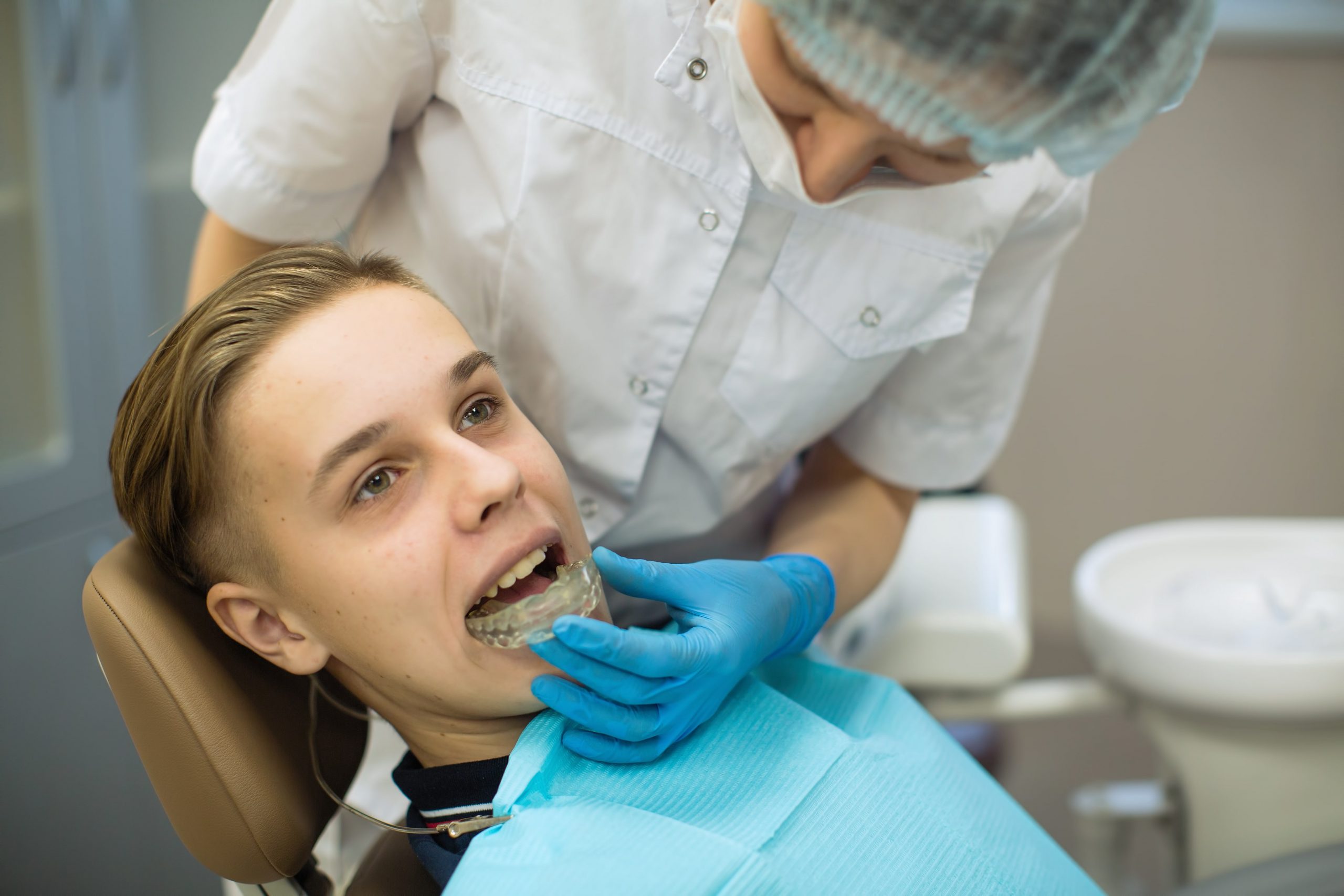
Treating patients with dental malocclusions requires careful evaluation and treatment planning. In this case study, after failing to correct a mandibular prognathism with aligners, a dentist refers the patient to an orthodontist. With the help of that orthodontist, an oral surgeon performs orthognathic surgery, but the procedures lead to root resorption. Later, the patient sues all three practitioners for negligence.
Key Concepts
- Importance of malocclusion evaluation for both skeletal and dental issues
- Risks of multiple defendant dentists who had treated the same patient
- Benefits of collaboration among dental professionals
Background Facts
T was a healthy 25-year-old man, 3 years out of college and trying to find his occupational path. T had excellent dental hygiene with a periodontium to match, but he had been bothered for years by what he often called his “Popeye jaw,” which he felt might be a factor in his repeated roadblocks in public-facing jobs. He discussed the issue with his longtime general dentist, Dr. G, who described the situation to T as a “large underbite.” Dr. G, who had recently completed a certification course given by a company that manufactured clear aligners, suggested placing those clear aligners, serially, to move the lower front teeth backward and the uppers forward, so that the lowers would be tucked under the upper front teeth. T agreed to the proposed plan, so treatment moved forward. But after a number of the serial aligners were placed and then replaced by the next in the series, T began to develop severe episodic bilateral jaw pain.
Unsure of what was taking place, Dr. G referred T to an orthodontist, Dr. O, with whom he had occasionally worked over the years. Upon seeing T, Dr. O took and then mounted an articulated set of study models, and obtained cephalometric and panoramic radiographs. Dr. O concluded that T’s problem was a skeletal malocclusion, caused by a combination of a prognathic mandible and a retrognathic maxilla, and not the dental malocclusion that Dr. G had begun to treat with aligners. Dr. O explained to T that she would need to place T in traditional orthodontic appliances to undo the severe tilting of the anterior teeth created by the aligners, which she believed to be the cause of the muscular pain T was experiencing. Dr. O further advised – with detailed explanation – that, after the teeth were “untilted” and a few rotated teeth were “unrotated,” T would need to be treated with orthognathic surgery to eliminate the skeletal-based bite issues.
T thought about Dr. O’s proposals for some time, getting opinions from family members and friends, some of whom encouraged him to go forward and others of whom discouraged it. But it was the ongoing discomfort that led T to take Dr. O’s treatment suggestion. Dr. O joined T and his father at the office of oral and maxillofacial surgeon, Dr. S. Dr. S wanted to review the diagnostics, in conjunction with intra- and extra-oral photographs that he took that day, so he asked everyone to reconvene 2 weeks later, at which time they would all discuss treatment options and potential risks. During that time period, Drs. O and S discussed T’s case and expressed their approaches to T and his father when they next met.
The plan presented was that Dr. O would perform the orthodontics just as she had earlier thought, after which Dr. S would perform a Le Fort I osteotomy to advance the maxilla and bilateral mandibular osteotomies to set that jaw back, thereby correcting the skeletal malocclusion. When the surgical sites healed, Dr. O would finish the process by making minor orthodontic movements to idealize the dental relationships vis-à-vis the “new” skeletal positioning.
Treatment went forward as expected, seemingly uneventfully. T’s pain resolved and he slowly returned back to his usual eating habits, with the approval of the treating doctors. However, his upper and lower anterior teeth were painful when he bit into hard foods like apples and bagels, and he became concerned about what he perceived as those teeth moving. When he returned to Dr. G for a recall exam and radiographs, it was discovered that he had a substantial amount of anterior root resorption that had never before existed prior to the whole course of treatment, which led Dr. G to refer T to a periodontist for evaluation. That periodontist completed a thorough periodontal assessment and then told T that the resorption was so significant – a fact that the periodontist found difficult to believe, given the relatively short treatment time – that he fully expected that T would lose between 6 and 8 of his 12 anterior teeth, likely within the next decade, if not sooner. T became extremely upset as he processed the likelihood of tooth loss and the costs that would accompany replacing them, plus the associated further delay in his career advancement.
Legal Action
T sought and hired an attorney who was a dental malpractice “regular.” The attorney obtained all of T’s relevant records and had them reviewed by experts in orthodontics and oral surgery. Both concluded that the root resorption resulted from the inappropriate and repeated (back and forth) forces placed on the anterior teeth, over a relatively short time. They were unable to conclude whether it was the treatment of Dr. G or Dr. O, or both, which caused the mobility and presumptive tooth loss. The oral surgery expert would not say that the orthognathic surgery made that condition worse, but did say that Dr. S’s failure to inspect the condition of the anterior teeth before doing surgery led to his performing surgery which, at the very least, delayed diagnosis of the root resorption, so that the need for extraction going forward became solidified.
T’s attorney instituted suit against all 3 of T’s treating practitioners, asserting different roles: Dr. G and Dr. O, by way of their respective orthodontic treatments, exerted inappropriate forces so as to directly lead to root resorption. Dr. S failed to timely identify the root resorption prior to performing surgery, thereby postponing the discovery of that condition beyond the time when periodontal care could have been instituted to improve the chances of those teeth surviving. In addition to claiming, as damages, the anticipated loss of teeth and the procedures, with their associated costs to replace them, T also claimed lost earnings because missing front teeth is a far greater stumbling block to career advancement than the initial skeletal malocclusion, according to his attorney.
Once the suit was reported to the malpractice carriers for Drs. G, O and S, each was assigned individual defense counsel. Unfortunately, but immediately, the attorneys for Drs. G and O began what would be a prolonged finger pointing exercise against each other’s clients, claiming it was the other defendant, and not their client, who was truly at fault for the severe root resorption. Among the few things all defense counsel could agree upon was the entirely speculative nature of the claim of T’s career advancement being stifled, in a man whose career was not going anywhere from the start. When presenting that argument to the court, the judge agreed and dismissed that portion of the claim.
With no pre-trial agreement able to be put together, the case proceeded to trial. With all 3 defendants presenting experts who defended the treatments, the jury found in favor of the oral surgeon, Dr. S, concluding that he played no role in the moving of the teeth – but only in the moving of the bones in which those teeth sat – and that there was insufficient evidence that any delay he might have caused had any substantial effect upon tooth loss. With Drs. G and O continuing to place blame on each other throughout the trial, the jury determined that it was impossible to know which portion of the root resorption was caused by each. But it was clear that each of them did play a negligent role in that result, so liability was split evenly between both.
Takeaways
Anytime there are multiple defendant dentists in a single case, a risk always exists that they might become adversarial and “unjoined” in their respective defenses. It is for that reason that separate defendants are often represented by separate attorneys, even if those defendant dentists are insured by the same carrier, unless the facts and personalities are such that there is an unwavering sense that their defenses will not be in conflict with each other to any extent at all.
This case might well raise the question as to why T’s future career activities were deemed impermissible due to speculation, while the prospect of future tooth loss was allowed to proceed in the case, as non-speculative. The answer lies with the background and underlying facts – a track record, if you will. Here, T had no employment or career track record, and his own initial presenting concerns included a lack of prior career advancement, so it would have been pure (impermissible) speculation to posit that, had the whole treatment course gone well, he would then have succeeded in some, as-yet-undetermined, career path. For context, contrast that with the non-speculative nature of an employee who is well entrenched in a job or profession, and loses income and/or opportunities due to negligent treatment. On the other side of the coin, experts in this case opined that multiple teeth, which now had objective, disadvantageous crown-to-root ratios because of root resorption, were likely to be lost prematurely, based upon dental evidence, clinically and radiographically, rendering it non-speculative. This is true even with disagreeing experts, because all would be basing their views on their opposing interpretations of scientific evidence.
While we generally stay away from assessing practitioners’ clinical judgments, it is clear from the facts of this case that Dr. G did not engage in a complete pre-orthodontic work-up before starting aligner therapy, which was far different from the work-up performed by Dr. O. Aligner therapy is rapidly gaining in popularity, but some dentists do not view it as the orthodontics that it truly is, so it is not given the degree of planning comprehensiveness that traditional orthodontics is.
We end with what might be taken as totally obvious. Dentistry often involves treatment of a patient by multiple dentists, whether simultaneously or in succession. When that is the situation, and results do not turn out as hoped or expected, there can be a tendency among those dentists to point a finger of blame against one another, rather than to work together to solve problems and lead patients to the best possible results. The value of the latter in idealizing patient care and in helping to avoid litigation cannot be overemphasized.
Note that this case presentation includes circumstances from several different closed cases, in order to demonstrate certain legal and risk management principles, and that identifying facts and personal characteristics were modified to protect identities. The content within is not the original work of MedPro Group but has been published with consent of the author. Nothing contained in this article should be construed as legal, medical, or dental advice. Because the facts applicable to your situation may vary, or the laws applicable in your jurisdiction may differ, please contact your personal or business attorney or other professional advisors if you have any questions related to your legal or medical obligations or rights, state or federal laws, contract interpretation, or other legal questions.
Additional Risk Tips content
OMS “Soft Sells” Risks of TMJ Surgery for A Locked Open Mandible
In this case study, a patient files a malpractice claim tied to informed consent, despite a successful surgery. Learn how communication affects risk.

Oral Surgeon Navigates the Gray Areas of Cosmetic Care
In this case study, a cosmetic facial treatment leads to a Board complaint against an OMS. Read the case to learn how scope of practice rules affect OMS.
Failure to Verify Leads to Irreversible Surgical Error
In this case study, wrong site oral surgery leads to malpractice claims. Read the article to learn how pre-procedure safeguards can prevent devastating errors.
This document does not constitute legal or medical advice and should not be construed as rules or establishing a standard of care. Because the facts applicable to your situation may vary, or the laws applicable in your jurisdiction may differ, please contact your attorney or other professional advisors if you have any questions related to your legal or medical obligations or rights, state or federal laws, contract interpretation, or other legal questions.
MedPro Group is the marketing name used to refer to the insurance operations of The Medical Protective Company, Princeton Insurance Company, PLICO, Inc. and MedPro RRG Risk Retention Group. All insurance products are underwritten and administered by these and other Berkshire Hathaway affiliates, including National Fire & Marine Insurance Company. Product availability is based upon business and/or regulatory approval and/or may differ among companies.
© MedPro Group Inc. All rights reserved.