Patient Must Cancel Joint Surgery Due to New Dental Guidelines
Marc Leffler, DDS, Esq.
November 26, 2025
Reading time: 7 minutes
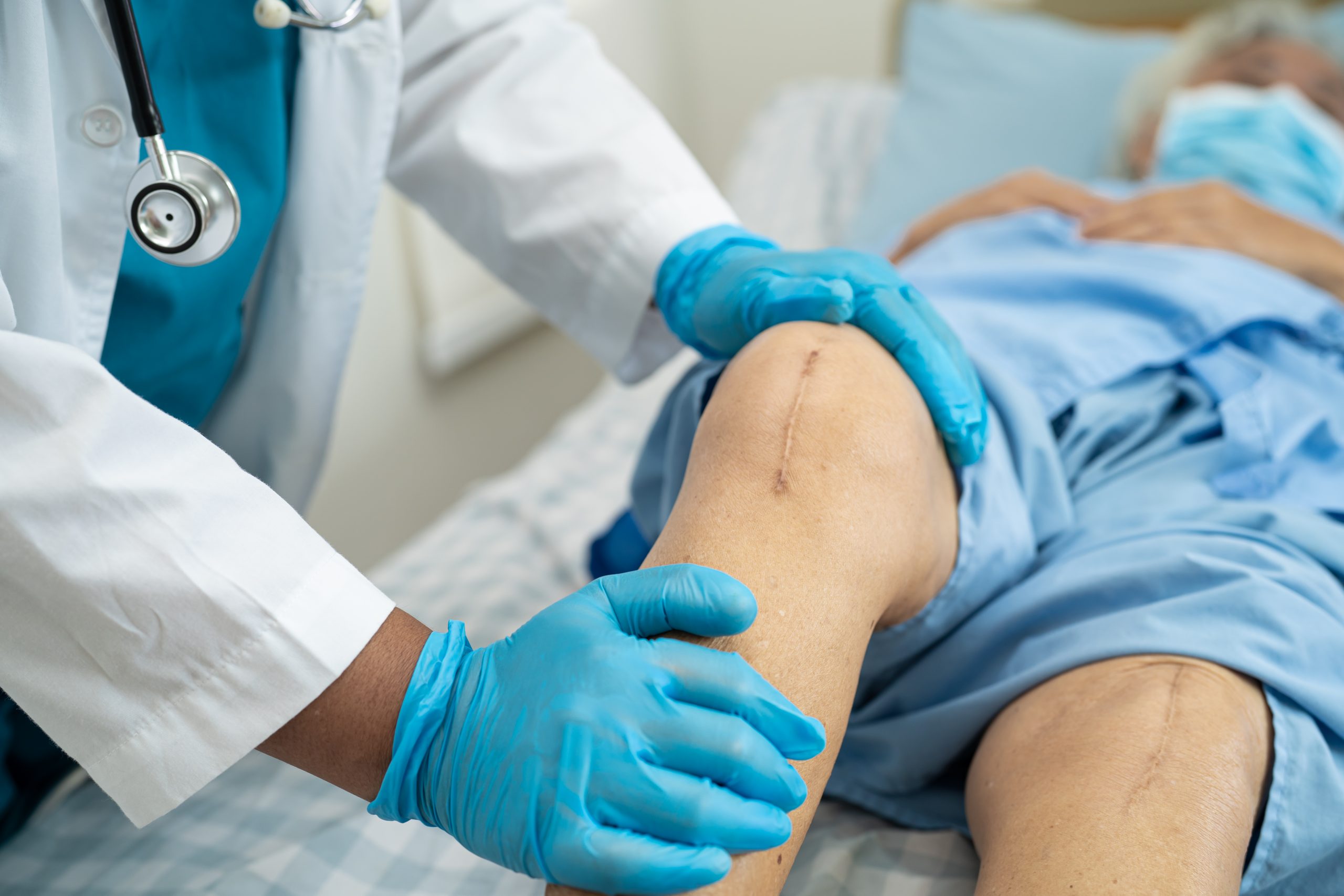
Considering recent guidelines regarding joint replacement surgeries, it’s more crucial than ever that oral surgeons coordinate their care with other medical professionals. In this case study, an oral surgeon performs multiple tooth extractions, unaware of the new guidelines surrounding the timing of dental procedures in relation to total joint arthroplasty (TJA). To reduce the risk of joint infection, the orthopedic surgeon reschedules the patient’s knee surgery for several months later. The patient expresses frustration at the inconvenience and the oral surgeon’s lack of awareness regarding these guidelines. However, no legal action is ultimately taken.
Key Concepts
- Staying informed on evolving dental guidelines
- Separating guidelines from standards of care
- Understanding protocols for patients with joint replacements
- Documenting communication between healthcare providers
Background Facts
P knew, from years of being told by various dental professionals, that he needed a number of teeth extracted due to gross decay. He admittedly did not have regular and adequate home oral hygiene habits, often leaving him with plaque build-up throughout his mouth and several areas of calculus, particularly on his lower anterior teeth. With an elective knee replacement surgery coming up in 2 weeks, he thought that this would be a good time to have those teeth extracted, in large part because he had read some online information about knee surgery and the potential for mouth bacteria to spread to that surgical site and lead to knee prosthesis loss.
When Dr. N examined P, clinically and radiographically, she noted 8 teeth in need of extraction, in addition to a long-overdue prophylaxis. P made Dr. N aware of the upcoming knee surgery. She arranged for P to have a cleaning that same day, with the extractions to be completed in 3 days.
The extractions went forward uneventfully, leaving a week-and-a-half before the scheduled orthopedic surgery. P saw Dr. N post-operatively to check the extraction sites, 5 days before the knee was to be treated, and all appeared to be healing within normal limits, although a lone bone spicule was easily removed.
P met with his orthopedic surgeon, Dr. C, in the hospital’s pre-surgical waiting area, where P casually mentioned that he had multiple dental extractions about 10 days prior, and the removal of a “small sliver of bone 5 days ago.” Dr. C immediately canceled the knee replacement surgery and told P to contact his office to reschedule once there would be no further dental intervention in those sites. At P’s request to understand more, Dr. C explained that current guidelines, which had “just taken effect,” included that there be a waiting period between oral surgery procedures and certain elective joint surgeries. Frustrated at the situation – because he had taken time off from work, asked family members to rearrange their own schedules to assist him upon his return home, would now need to redo his pre-operative lab testing, and would have to again go through the stress in anticipation of surgery. P contacted Dr. N’s office, asking to come in immediately.
Dr. N was surprised to see P, expecting that he would have been hospitalized and under his orthopedic surgeon’s care. P angrily explained what had happened, with Dr. N listening intently. Dr. N said that she had been unaware of any protocols in place that would have led Dr. C to cancel surgery for a dental-based reason. Nevertheless, she apologized profusely, but P never returned to see her. P located another dental practitioner, who determined the extraction sites to be completely healed, roughly a month or so later. P underwent successful knee replacement surgery, albeit several months after initially planned, with no complications.
Legal Action
Still upset over the entire episode, P spoke with a cousin who is an attorney, as well as a local medical malpractice lawyer. Both gave him the same advice, namely that, although he had suffered from significant inconvenience due to Dr. N’s lack of knowledge, he had no damages which would reasonably be compensable. The second attorney also pointed out that, even if Dr. N had been aware of the new protocol, the teeth were quite likely in need of extraction before the joint surgery anyway, so the orthopedist would have postponed the procedure in any event. All of P’s frustrations would have, therefore, been essentially the same.
Understanding that suing Dr. N would only be able to happen if he represented himself, P sent her a letter requesting copies of his entire chart, and asking her to report the incident to her malpractice carrier, which she did. No further action was ever taken by P.
Takeaways
The “current guidelines” referenced by Dr. C came into effect in late 2024, by way of protocols jointly developed by the American Academy of Orthopedic Surgeons (AAOS), the American Dental Association, and several other organizations. By way of history, the use of antibiotics in association with dental procedures for patients with joint replacements was recommended until as recently as approximately 2012, when the guidance changed to consider discontinuing that practice. The current approach regarding the relationship between dentistry and joint replacements takes antibiotics out of the picture, and instead speaks to the timing of certain dental procedures, both before elective total joint arthroplasty (TJA) and after any TJA. The organizations involved carefully referred to them as guidelines, as compared with standards of care (SOC). But in a litigation setting, it is far from unforeseeable that an expert for a plaintiff might well incorporate the guidelines into their testified-to SOC, if the guidelines were not followed and a negative event ensued.
The new guidelines, briefly stated, are: (1) noninvasive and minimally invasive dental procedures can be performed until the day before elective TJA; (2) dental extractions and other oral surgery procedures should be completed at least 3 weeks before elective TJA (because they can be expected to take up to 3 weeks to heal); and (3) most dental procedures should be delayed – if possible – for 3 months after TJA. The goal, according to the co-chair of the guideline group, is to prevent infections that might emanate from dental procedures, due to bacterial entrance into the bloodstream, which can then attach to the new joint prosthesis, thereby infecting it.
Even though litigation never took place in this case study, it would not be unexpected to imagine that litigation might well have gone forward if the result to P were different. For example, if P had the TJA and then presented to Dr. N 1-2 months later, and if Dr. N had performed the extractions at that time (with both P and Dr. N unaware of the new guidelines), and if the joint prosthesis were then lost to infection due to bacteria commonly found in the mouth, an expert for P, as plaintiff, would be able to make a colorable argument that P suffered as a result of Dr. N not following a published guideline, namely the waiting for 3 months after the TJA to extract the teeth.
A fair reading of the guidelines leaves some room for interpretation, such as what constitutes “noninvasive and minimally invasive dental procedures,” and what dentistry fits under the umbrella of “most dental procedures.” If unclear, a risk-protective approach is to directly involve the orthopedic surgeon, explaining what dentistry is planned, so that the surgeon replacing the joint can have input into the plan of action. In such situations, documentation of those communications is critical, in the event that a lawsuit or Board action were to later arise. A written plan – a letter, email, or text message – from the orthopedist is ideal, but absent that, a detailed, contemporaneous entry by the dentist/oral surgeon into the patient’s chart will serve as a solid, if not perfect, memorialization.
With dentistry and medicine fronts expanding at a fast pace, and with technology fueling that expansion, sometimes seemingly overnight, the burdens upon dental professionals to stay up to date about all aspects of patient care can be daunting. But that is exactly what is required to practice within the standard of care. The fact that a dentist might not be aware of very recent, yet relevant, changes that directly affect their practice will not serve to excuse any lapses that occur as a result. An approach looked at today as up-to-date might be viewed as old-fashioned and outdated tomorrow. Here, although Dr. N was made aware of P’s upcoming knee replacement surgery, she was not aware of the potential impact of her planned dental treatment upon that surgery. That directly and negatively affected P, but fortunately, in not very significant ways.
A question to consider is whether the patient, P, bears any responsibility for the events in this case, particularly by allowing his teeth to fall into such disrepair, all at his own hand, and for waiting until the virtual eve of knee surgery before seeking to address his dental problems. States vary in their handling of this type of issue during the course of litigation. But even when a particular jurisdiction allows for claims by the defendant against the plaintiff that might greatly reduce or completely eliminate monetary compensation, it becomes a strategic question for defense counsel (and the dentist’s malpractice carrier) as to whether there is value in going down that road, with the specter of the potential for a jury to be angered by the attempt to “blame the victim.” Litigation is a process that includes facts, law, strategy, ethics, and assessments of human nature, complex and intellectually stimulating.
Note that this case presentation includes circumstances from several different closed cases, in order to demonstrate certain legal and risk management principles, and that identifying facts and personal characteristics were modified to protect identities. The content within is not the original work of MedPro Group but has been published with consent of the author. Nothing contained in this article should be construed as legal, medical, or dental advice. Because the facts applicable to your situation may vary, or the laws applicable in your jurisdiction may differ, please contact your personal or business attorney or other professional advisors if you have any questions related to your legal or medical obligations or rights, state or federal laws, contract interpretation, or other legal questions.
Additional Risk Tips content
OMS “Soft Sells” Risks of TMJ Surgery for A Locked Open Mandible
In this case study, a patient files a malpractice claim tied to informed consent, despite a successful surgery. Learn how communication affects risk.

Oral Surgeon Navigates the Gray Areas of Cosmetic Care
In this case study, a cosmetic facial treatment leads to a Board complaint against an OMS. Read the case to learn how scope of practice rules affect OMS.
Failure to Verify Leads to Irreversible Surgical Error
In this case study, wrong site oral surgery leads to malpractice claims. Read the article to learn how pre-procedure safeguards can prevent devastating errors.
This document does not constitute legal or medical advice and should not be construed as rules or establishing a standard of care. Because the facts applicable to your situation may vary, or the laws applicable in your jurisdiction may differ, please contact your attorney or other professional advisors if you have any questions related to your legal or medical obligations or rights, state or federal laws, contract interpretation, or other legal questions.
MedPro Group is the marketing name used to refer to the insurance operations of The Medical Protective Company, Princeton Insurance Company, PLICO, Inc. and MedPro RRG Risk Retention Group. All insurance products are underwritten and administered by these and other Berkshire Hathaway affiliates, including National Fire & Marine Insurance Company. Product availability is based upon business and/or regulatory approval and/or may differ among companies.
© MedPro Group Inc. All rights reserved.