Communication Mishap Between Providers Leads to Wrong-Site Extraction
Case Study
Marc Leffler, DDS, Esq.
July 28, 2025
Reading time: 8 minutes
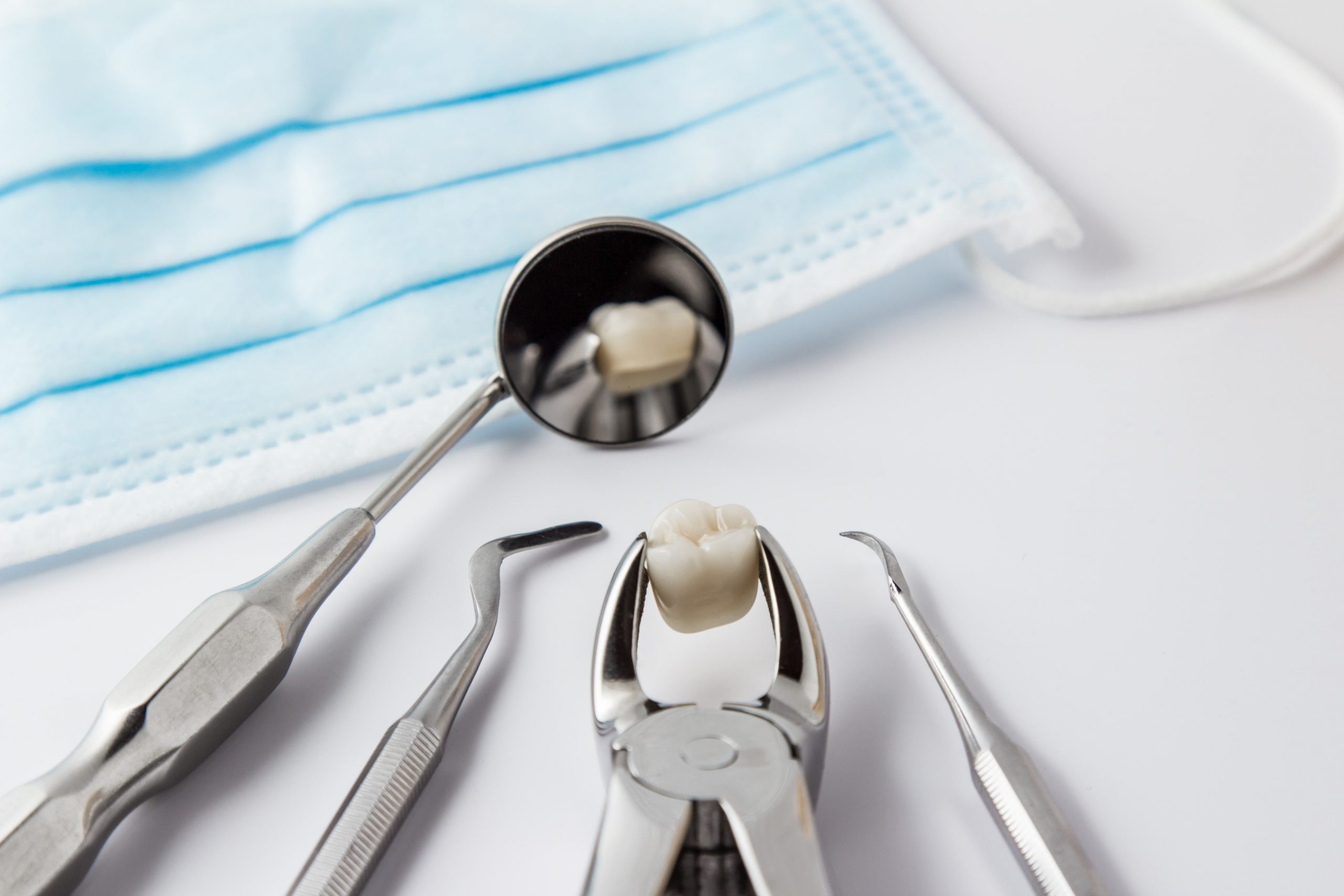
Proper communication between dental providers is essential when referring a patient for a procedure. In this case study, a patient is referred to an oral surgeon for a tooth extraction, but a miscommunication with the referring dentist causes the oral surgeon to extract the wrong tooth.
Key Concepts
- Extraction of incorrect tooth
- Dental numbering systems
- Staff education
Background Facts
An 18-year-old high school senior began April 1st by receiving the invitation to her upcoming prom that she had been hoping for; at first, she thought the question was an April Fools’ joke, but it was not. After school that day, she went to her previously scheduled dental visit to address 2 issues: a periodically painful impacted upper right third molar, and a supragingivally fractured upper right central incisor that had been struck by a softball a few months prior. Her general dentist clinically and radiographically examined her mouth, with focus on the areas of concern. He determined that the wisdom tooth ought to be extracted because its angulation prevented eruption, after which he would restore the central incisor (before prom night). Sarah wanted to move things along quickly, so she agreed to head to the oral surgeon the same day for the extraction, even though she was nervous about having her tooth extracted; because she had not eaten anything after breakfast, she could be sedated.
Dr. G instructed the office manager to call the oral surgeon’s office to ask whether they could see Sarah to “extract the upper right #8”. The office manager spoke with Dr. O’s receptionist, used Dr. G’s exact words, and was told to “send her over now”. No written referral form or radiograph was given to Sarah to deliver to Dr. O. When she arrived at Dr. O’s office with her mother, Sarah provided a benign medical history, and then signed a “consent form for extraction of ‘upper tooth’” while she sat in the waiting room. A panoramic film was then taken, and Sarah was seated in a treatment room. Dr. O briefly introduced himself to Sarah, reviewed her medical history, looked at the panoramic and the handwritten entry on the day sheet to “extract the upper right #8”, and injected sedative medication intravenously.
Once Sarah was sedated, Dr. O remarked to his assistant how unaesthetic the upper right central incisor appeared due to the sports accident. He gave an upper anterior buccal infiltration of local anesthetic and routinely extracted the upper right central incisor. When Sarah’s mother came into the recovery room, she immediately saw that the front tooth had been extracted and began to cry. As Sarah listened to her mother, she thought it was an April fools’ joke, but it was not. Dr. O became very upset when he heard Sarah’s mother and found out why she was crying, and immediately called Dr. G: it was then that he learned that Dr. G had sought the extraction of the upper right third molar (UR8) rather than the upper right central incisor (tooth #8), the latter of which he planned to cosmetically restore. Both dentists agreed to work together to provide Sarah with an implant at the site of tooth #8 and a crown upon it, all at no charge. That treatment was ultimately carried out, but not before the prom, so Sarah attended wearing a flipper, feeling very self-conscious.
Legal Action
Shortly after that treatment was completed, Sarah’s newly retained attorney filed a dental malpractice lawsuit against Drs. G and O. The claim against Dr. G was essentially that he had negligently failed to properly communicate to Dr. O the treatment plan he wanted to be carried out. The allegations against Dr. O were that he extracted the wrong tooth because he delegated the interactions with Dr. G’s office solely to non-dental office staff, failed to obtain informed consent for the procedure he performed, and failed to perform the level of patient assessment necessary for this patient’s treatment. Although Sarah had no out-of-pocket expenses for the initial implant placement and restoration, her new general dentist advised her that she may well need to have the implant replaced at least once or twice, and very likely need to have the crown redone every 10-15 years. The suit sought compensation for the projected future dental costs, as well as the emotional distress she suffered and would continue to endure.
Discovery and Case Resolution
From the early days of the lawsuit, Dr. O acknowledged his errors and his desire to try to “make things right” for Sarah, so he encouraged the attorneys provided by his malpractice insurance carrier to settle the case by appropriately compensating Sarah. However, Dr. G did not see it the same way, believing that, in the end, the responsibility lies with the dentist actually performing the extraction to make sure that the proper tooth is extracted. So, at his deposition, Dr. G placed the entire blame on his oral surgery colleague – a concept referred to as “jousting” – and then exercised his malpractice policy provision which permitted him to refuse a settlement on his behalf.
Sarah and her attorney accepted the settlement offer on behalf of Dr. O and prepared to go to trial against Dr. G alone. But as that date approached, Dr. G ultimately decided that the stress and lost time from practice were not in anyone’s best interests, so he agreed to allow his carrier to make a settlement payment on his behalf, thereby ending the case.
Takeaways
Here, as in many dental malpractice circumstances, there are multiple factors which led to the improper treatment of this patient; had any one of those elements been realized and eliminated from the chain, Sarah would have had her wisdom tooth removed and her central incisor restored.
It is far from uncommon for non-dental office staff members to play critical roles in untoward outcomes, whether by misinterpreting what is said to them and passing on that incorrect information to patients or other providers or giving dental or medical advice to patients without a dentist’s knowledge or input, or making scheduling changes which delay time-sensitive treatment. Non-dental staff are not aware of nuances relating to patient care to a degree adequate to allow for significant decision making, but their actions are legally attributed to their dentist employers, so dentists are wise to realize this and, therefore, closely monitor the actions of staff. In this situation, neither Dr. G’s office manager nor Dr. O’s receptionist likely understood the multiple – and sometimes confusing – ways that teeth are numbered, directly leading to the first mistake. Both Drs. G and O bear legal liability for the actions of their employees.
When Dr. O saw the handwritten schedule entry of “extract the upper right #8”, he could have broken the error chain by considering what he clearly knew: that there are at least 3 tooth numbering systems in use – the universal system (#1-32), the Palmer system (quadrants of upper right, upper left, etc. with teeth numbered in each quadrant from 1-8 moving back from the midline), and the FDI system (referring to the quadrants in clockwise fashion from 1-4 and numbering the teeth from 1-8 in each numbered quadrant as in Palmer). So, the upper right third molar can be referred to as #1, UR8, or 18 (not to be confused with the lower left second molar, #18), respectively, and the upper right central incisor can be called #8, UR1, or 11 (not to be confused with the upper left canine, #11), respectively. There is no getting around the fact that these classifications are easily and often mixed up, complicated by the vintage and geography of the individual dentists involved. So, before performing any invasive dental procedure, especially when a referral is involved, it behooves the referring dentist and the referred-to dentist to be 100% certain of the tooth to be worked on.
Had Dr. G taken the time to send a written communication of the desired treatment to Dr. O or had Dr. O taken the time to call Dr. G before starting treatment, or had some combination of those actions taken place, the mistake would have been averted. Furthermore, had Dr. O not limited the informed consent process to simply giving the patient a form to sign in the waiting room, and delegated the potential back-and-forth discussion to front desk personnel, but instead fully discussed the treatment with Sarah before the sedation began, the mistake would have been averted.
Dentists have lagged well behind their medical colleagues in the consistent taking of a “time out” prior to the start of invasive procedures. That process, which takes only a short time, involves the input of the entire procedure team to assure the correct patient, the correct procedure, the correct site, the correct side, and any other specific precautions determined by the person in charge to be prudent. The importance of a “time out” cannot be overstated in its effectiveness in preventing wrong-site surgery: a retrospective study of non-emergent surgeries at Vanderbilt Medical Center in 2016, and published in the journal Anesthesia & Analgesia in 2020, found that there had been no wrong-site or wrong-person surgeries when a “time out” – averaging less than one minute in duration – had been taken prior to incision; a JAMA Network publication from 2018 reported 95 wrong-patient, wrong-site, or wrong-procedure operating room events in VA facilities during 2017, all taking place with no “time out” or a faulty “time out”, with dentistry leading the way in this undesirable statistic among all healthcare practice areas. Had a “time out” been taken here, the mistake would likely have been averted.
As with so many aspects of dental practice, proper, timely and clear communication plays an important and indispensable role in avoiding untoward events which often lead to malpractice and the litigation to obtain compensation for it. It cannot be denied that some practices function on the speedy treatment of patients, with the dentists practicing there being pressured to fall in line, but those are the situations most vulnerable to the types of entirely avoidable errors discussed in this case study.
Note that this case presentation includes circumstances from several different closed cases, in order to demonstrate certain legal and risk management principles, and that identifying facts and personal characteristics were modified to protect identities. The content within is not the original work of MedPro Group but has been published with consent of the author. Nothing contained in this article should be construed as legal, medical, or dental advice. Because the facts applicable to your situation may vary, or the laws applicable in your jurisdiction may differ, please contact your personal or business attorney or other professional advisors if you have any questions related to your legal or medical obligations or rights, state or federal laws, contract interpretation, or other legal questions.
Additional Risk Tips content
OMS “Soft Sells” Risks of TMJ Surgery for A Locked Open Mandible
In this case study, a patient files a malpractice claim tied to informed consent, despite a successful surgery. Learn how communication affects risk.

Oral Surgeon Navigates the Gray Areas of Cosmetic Care
In this case study, a cosmetic facial treatment leads to a Board complaint against an OMS. Read the case to learn how scope of practice rules affect OMS.
Failure to Verify Leads to Irreversible Surgical Error
In this case study, wrong site oral surgery leads to malpractice claims. Read the article to learn how pre-procedure safeguards can prevent devastating errors.
This document does not constitute legal or medical advice and should not be construed as rules or establishing a standard of care. Because the facts applicable to your situation may vary, or the laws applicable in your jurisdiction may differ, please contact your attorney or other professional advisors if you have any questions related to your legal or medical obligations or rights, state or federal laws, contract interpretation, or other legal questions.
MedPro Group is the marketing name used to refer to the insurance operations of The Medical Protective Company, Princeton Insurance Company, PLICO, Inc. and MedPro RRG Risk Retention Group. All insurance products are underwritten and administered by these and other Berkshire Hathaway affiliates, including National Fire & Marine Insurance Company. Product availability is based upon business and/or regulatory approval and/or may differ among companies.
© MedPro Group Inc. All rights reserved.